When you hear the term dementia, Alzheimer's disease is the one that comes to your mind. But there is a second. Often underdiagnosed... a form of dementia that affects around 8.5 million people worldwide… known as vascular dementia (VaD).
VaD represents vascular cognitive impairment, which is mainly caused by brain blood flow reduction. It is a progressive neurological condition. It erodes memory & rational reasoning. Also compromises your ability to carry out everyday tasks.
Alzheimer's and vascular dementia differ, as vascular dementia is partly preventable and partly manageable. And this factor makes the makes early recognition and action by dementia care specialists critically important.
What Is Vascular Dementia?
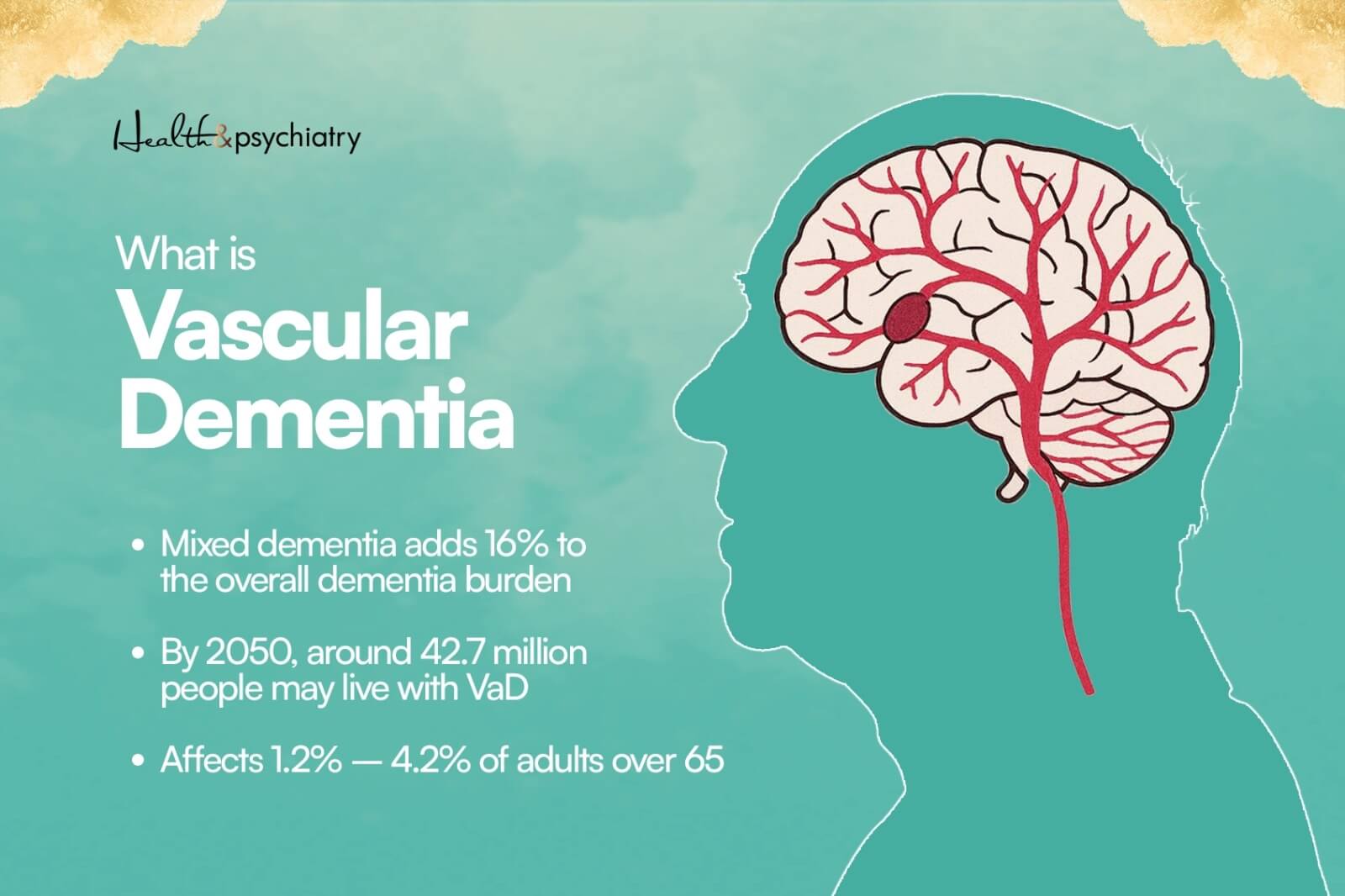
Vascular dementia is a broad term used to describe cognitive decline. It happens due to conditions that damage the blood vessels supplying the brain. Brain blood flow reduction becomes a reason for vascular cognitive impairment.
Maybe through a stroke, or a series of mini-strokes, TIAs (transient ischemic attacks), or progressive narrowing of small vessels, the blood flow reduction causes brain tissue to be deprived of oxygen and nutrients. This damage accumulates over time. It then begins to impair thinking, memory, and daily functioning.
Vascular dementia can occur on its own. And also alongside other types of dementia. Most notably, Alzheimer's disease. When both pathologies are present, it is referred to as mixed dementia. Quite common it is!
Key vascular dementia statistics by the World Stroke Organization show that Vascular dementia is the second leading cause of all dementia worldwide.
- An 16% addition to the overall burden is caused by mixed vascular and degenerative dementia.
- The global VaD burden is expected to become 42.7 million people living with vascular dementia, by 2050… if current trends continue.
- Prevalence ranges from 1.2% to 4.2% in adults over age 65, varying by country
- These numbers underscore both the scale of this condition and the urgent need for awareness, early diagnosis, and evidence-based care.
What Causes Vascular Dementia?
Major causes of vascular dementia (VaD) are:
1. Stroke (Major or Repeated Small Strokes)
One of the most common causes of vascular dementia is Stroke. When blood flow to a part of the brain is suddenly blocked. Or when a blood vessel bursts, it occurs. Leading to immediate brain cell damage.
Even smaller strokes, known as TIAs (Transient Ischemic Attacks) or “mini-strokes,” can cause it. Not obvious symptoms at first. But repeated episodes can gradually damage brain tissue and affect memory and thinking.
2. Small Vessel Disease
Small vessel disease affects the tiny blood vessels. Deep inside the brain. These vessels become narrowed, stiff, or damaged over time. Thus, reducing blood flow to important brain regions.
This slow and continuous restriction of oxygen and nutrients can lead to progressive cognitive decline.
3. Chronic Medical Conditions
Several long-term health conditions can be a cause of vascular dementia.
- High blood pressure is the strongest risk factor for vascular dementia. It weakens and damages blood vessels over time.
- Diabetes, when poorly controlled, contributes to damaging small blood vessels. It can also increase inflammation.
- Heart conditions, especially atrial fibrillation, can cause blood clots that travel to the brain.
- High cholesterol also plays a role by narrowing arteries. It reduces circulation.
4. Lifestyle Factors
Lifestyle and your habits significantly influence vascular health.
If you smoke, it can damage blood vessel walls. It can also increase clot formation.
If you have a sedentary lifestyle, a poor diet, obesity, and excessive alcohol intake? Beware! As they all contribute to poor circulation. Causing a higher risk of stroke and vascular damage over time.
5. Genetic and Rare Conditions
Genetic disorders like CADASIL (cerebral autosomal dominant arteriopathy with subcortical infarcts and leukoencephalopathy) affect the structure of small brain blood vessels. Although rare, but it is a cause of vascular dementia.
As it leads to reduced blood flow at an earlier age and can cause early-onset vascular dementia.
Stages of Vascular Dementia
Alzheimer's disease follows a gradual decline. a more predictable one. But unlike that, vascular dementia often progresses in a stepwise fashion. No sudden decline. But a relatively gradual loss.
While there is no formal staging system for vascular dementia, experts universally agree on one.
Typically, these vascular dementia stages are described by clinicians to explain this illness:
1. Early Stage (Mild Vascular Dementia)
For people living with vascular dementia, the early stages represent subtle cognitive changes. They may easily attribute it to normal aging or stress.
Generally, in the early stages of VaD, a person is still independent.
May begin to notice:
- Concentrating or focusing on a task becomes difficult.
- Processing speed & thinking become slower.
- Mild confusion, especially in unknown environments.
- Planning & doing tasks involving multi-step become tough. (e.g., cooking a recipe, managing finances).
- Mild memory difficulties
- Mood changes. Can cause depression, anxiety, or emotional lability.
On this stage, closer ones and family members begin to notice changes. That the person is taking longer to complete tasks. Or is becoming more forgetful of appointments. Or seeming more irritable or withdrawn.
2. Middle Stage (Moderate Vascular Dementia)
Vascular dementia progresses. The deficits become more pronounced. Beginning to significantly affect daily independence:
- Greater memory impairment. Recent chats and events are no more remember.
- Problem-solving and making judgments become tougher.
- Communication difficulties start with noticeable vascular dementia personality changes.
- Comes with a struggle to find words or follow conversations.
- Getting lost in familiar places.
- All this increasing dependence on others. Compromising dressing, personal hygiene.
- Behavioral changes. Causing agitation, vascular dementia anger, depression or social withdrawal.
- Possible hallucinations in some patients.
- Physical changes. Including gait instability, shuffling walk, or urinary incontinence
This stage causes attention from caregivers, and proper consultation and treatment under a vascular dementia specialist.
3. Late Stage (Severe Vascular Dementia)
 In the more progressed and severe stage, the person requires comprehensive support. Including the supervision for all daily activities:
In the more progressed and severe stage, the person requires comprehensive support. Including the supervision for all daily activities:
- Severe memory loss. The person may not recognize close family members.
- Minimal or no verbal communication.
- Full dependence for personal care, eating, and mobility.
- High risk of falls. Infections (particularly aspiration pneumonia) & pressure injuries.
- Significant swallowing difficulties (dysphagia).
- Loss of bladder and bowel control.
Palliative care and hospice planning become appropriate considerations at this stage of vascular dementia…
Key Symptoms of Vascular Dementia
Vascular dementia symptoms vary. Depending on the area and extent of brain damage. May be appearing suddenly after a stroke. May be develop gradually over time.
Cognitive Symptoms
These are often the earliest signs. Affecting thinking abilities:
- Slowed thinking.
- Reduced processing speed.
- Difficulty with tasks like planning, organizing, and decision-making.
- Problems with attention and concentration causing anger issues.
- Mild to moderate memory loss.
- Language difficulties. Such as trouble finding words.
- Disorientation to time and place.
Physical Symptoms
Vascular dementia presents with more physical changes than any other type of dementia. Noticeable physical changes in VaD are:
- Unsteady gait. Shuffling walk. Balance issues.
- Increased risk of falls.
- Weakness or numbness (often after a stroke).
- Urinary urgency or incontinence.
- Swallowing difficulties in later stages.
- Muscle stiffness or tremors in some cases.
Behavioral & Emotional Symptoms
Vascular dementia anger is a common issue. It comes with physical as well as cognitive decline. Causing irritation and aggressiveness while making progress. Challenging for both: a person living with vascular dementia and their caregivers.
Behavioural symptoms of Vascular dementia include:
- Depression and anxiety.
- Apathy and social withdrawal.
- Mood swings. Emotional instability (sudden crying or laughing).
- Irritability, agitation, and anger outbursts.
- Personality changes. (e.g., becoming suspicious or withdrawn).
- Sleep disturbances. Can cause insomnia or daytime drowsiness.
Early recognition of these symptoms and consultation with a dementia care specialist helps in better management and caregiver support.
Health & Psychiatry are trusted mental health care providers. We offer support from expert dementia care specialists in Florida. Providing personalized, compassionate care for individuals living with dementia….
How Is Vascular Dementia Diagnosed?

Vascular dementia diagnosis is a multi-step process conducted by a dementia care specialist. There is no single test that confirms it.
Instead, psychiatric assessment is done by a combination of medical history. Cognitive function and brain imaging to identify vascular cognitive impairment caused by brain blood flow reduction.
Steps involved in vascular dementia diagnosis are:
1. Medical and Cognitive History
Doctors begin by evaluating your symptoms. Their onset & progression are studied. A history of stroke or cardiovascular disease is especially important when determining what causes vascular dementia.
Input from family members is very helpful here. It is to identify subtle vascular dementia symptoms… including memory issues and vascular dementia personality changes.
2. Cognitive Testing
Standard tools like MoCA (Montreal Cognitive Assessment) and MMSE (Mini-Mental State Exam) are used. They are to assess thinking, memory, and problem-solving abilities.
Difficulties with planning, attention, and processing speed are often more prominent than memory loss in the early stages of vascular dementia.
3. Brain Imaging
MRI or CT scans play a key role in confirming the diagnosis. These scans can detect prior strokes. Also the white matter damage or other abnormalities that are somehow linked to reduced blood flow.
Imaging findings help distinguish what is vascular dementia from other conditions like Alzheimer’s.
4. Laboratory Tests
Blood tests are performed. For ruling out other causes of cognitive decline. Such as vitamin deficiencies or thyroid disorders. Well, it can also identify vascular dementia risk factors like diabetes or high cholesterol.
5. Cardiovascular Assessment
Since vascular dementia is closely tied to heart and blood vessel health. A dementia care specialist evaluates blood pressure, heart rhythm (ECG), and circulation during diagnosis procedures.
Managing these factors is essential for effective vascular dementia treatment.
6. Differentiating from Alzheimer’s Disease
Although symptoms may overlap… But vascular dementia often has a sudden or stepwise onset. While Alzheimer’s progresses gradually. Executive dysfunction appears earlier in vascular dementia. Whereas Alzheimer’s depicts memory loss more prominently.
How Does Vascular Dementia Progress?

The progression of vascular dementia varies. Depending on the underlying cause and overall health of the individual.
→ Gradual decline: Slow and continuous deterioration. Often seen in small vessel disease.
→ Stepwise decline: Sudden worsening after strokes or mini-strokes. Followed by periods of stability…
In a stepwise manner, the seven stages of dementia show a timeline of vascular dementia before death. They describe the gradual progression of cognitive decline. Ranging from normal functioning to severe impairment.
Seven Stages of Dementia
|
Stage |
Description |
Key Features |
|
Stage 1 |
No Cognitive Decline |
Normal memory and functioning; no symptoms. But changes in brain have already started. |
|
Stage 2 |
Very Mild Decline |
Minor forgetfulness (misplacing items, forgetting names). |
|
Stage 3 |
Mild Cognitive Decline |
Noticeable memory lapses, difficulty concentrating, and early confusion come with vascular dementia anger. |
|
Stage 4 |
Moderate Decline (Mild Dementia) |
Trouble with finances, planning, and recent memory. |
|
Stage 5 |
Moderately Severe Decline |
Needs help with daily tasks, disoriented, and forgets personal details. Physical changes start with dependency. |
|
Stage 6 |
Severe Decline |
Major memory loss, personality changes, requires assistance with basic care. |
|
Stage 7 |
Very Severe Decline |
Loss of speech, mobility, and full dependence on caregivers. |
These seven stages of vascular dementia may not always follow a perfectly smooth progression. Instead, individuals may move through stages unevenly. Especially if additional vascular events (like strokes) occur.
Treatment Options for Vascular Dementia

There is currently no cure or official treatment for vascular dementia. Nor have any medications been specifically approved by the FDA for its treatment.
However, there is always a comprehensive multidisciplinary approach at specialized facilities for dementia care. They can significantly impact the quality of life. Making things better for VAd person and their families.
Vascular dementia treatment focuses on slowing disease progression & preventing further vascular events.
It includes:
1. Managing Underlying Risk Factors
The most important part of VaD treatment is to control those conditions that can contribute to vascular cognitive impairment:
- Blood pressure control (key to preventing further damage).
- Managing diabetes and blood sugar levels.
- Lowering cholesterol.
- Treating heart conditions such as atrial fibrillation.
- Preventing future strokes.
If these factors are effectively managed, one can significantly improve vascular dementia prognosis and slow disease progression.
2. Medications
While there is no specific cure. Neither any FDA-approved vascular dementia medications..
- But certain Alzheimer's medications e.g., cholinesterase inhibitors, used off-label may help manage symptoms.
- Antiplatelet or anticoagulant medications to reduce stroke risk.
- Medications for depression, anxiety, or managing vascular dementia anger.
- Blood pressure and cholesterol-lowering drugs.
Medication plans are usually personalized… based on individual needs.
3. Lifestyle Modifications
Healthy lifestyle choices play a major role in treatment:
- Regular physical activity improves blood circulation.
- A heart-healthy diet (low in salt, saturated fats, and processed foods).
- Smoking cessation and limiting alcohol intake.
- Maintaining a healthy weight.
These changes support both brain and cardiovascular health.
4. Cognitive and Rehabilitation Therapies
Supportive therapies help maintain independence and function:
- Cognitive Rehabilitation Therapy (CRT) to improve memory and problem-solving.
- Occupational therapy (OT) to assist with daily tasks.
- Speech and Language Therapy (SLT) if communication is affected.
These interventions provide essential cognitive health support.
5. Behavioral and Emotional Support
Managing mood and behavior is crucial:
- Psychological support for depression, anxiety, and mood swings.
- Structured routines to reduce confusion and agitation.
- Caregiver education to manage vascular dementia personality changes effectively.
6. Long-Term Care and Support Services

As the condition progresses, patients may require increasing care:
- In-home care or assisted living support.
- Guidance from a vascular dementia specialist.
- Access to professional services for comprehensive management.
Looking for dementia care Florida providers? Consult with the expert team at Health & Psychiatry to get professional care for mental health management!
Although vascular dementia cannot be reversed… But an early intervention and a combination of vascular dementia treatment options can slow decline. It can reduce complications & improve the quality of life for those living with vascular dementia and their families.
Can Vascular Dementia Be Prevented?
Vascular dementia is unique among the dementias… How? Because it is partly preventable!
The reason is that many of its underlying drivers, including high blood pressure, diabetes, high cholesterol, smoking, obesity, and physical inactivity, are modifiable.
Interventions targeting these risk factors offer real opportunities to reduce the incidence and delay the onset of vascular dementia.
The 2024 Lancet Commission on Dementia Prevention, Intervention, and Care identified 14 risk factors of dementia that can be modified. They can together reduce overall dementia risk by up to 45%.
Many of these risk factors, including hypertension, diabetes, smoking, physical inactivity, obesity, and hyperlipidemia, are directly relevant to vascular dementia.
Effective prevention strategies include:
 → Control Blood Pressure. Maintain your systolic blood pressure below 130 mmHg. It is one of the most effective ways to reduce vascular damage. Also to lower the risk of stroke.
→ Control Blood Pressure. Maintain your systolic blood pressure below 130 mmHg. It is one of the most effective ways to reduce vascular damage. Also to lower the risk of stroke.
→ Manage Diabetes. Always keep your blood sugar levels under control. Through medication, if you are diabetic. Diet and exercise help prevent damage to small blood vessels in the brain.
→ Lower Cholesterol. Reduce plaque buildup in arteries and improve circulation via a balanced diet or medications (prescribed by a doctor).
→ Quit Smoking. Everyone knows smoking damages blood vessels. Increasing clot formation… You need to stop smoking at any stage to reduce vascular risk.
→ Exercise Regularly. The average recommendation is engaging in at least 150 minutes of moderate aerobic activity per week. It is to improve heart health and enhance blood flow to the brain.
→ Maintain a Healthy Weight. If you engage in managing body weight, it will help you to reduce the risk of hypertension, diabetes, and high cholesterol-related diseases.
→ Limit Alcohol Intake. Excessive alcohol consumption may lead to alcohol abuse, increasing blood pressure, mental health issues & stroke risk. So moderation is essential!
→ Manage Heart Conditions. Timely treatment of conditions like atrial fibrillation helps prevent blood clots. As they can lead to stroke.
→ Regular Health Check-Ups. Routine medical visits allow early detection and management of vascular dementia risk factors. Improving long-term outcomes.
Risk Factors for Vascular Dementia
Vascular dementia risk factors fall into two broad categories: non-modifiable and modifiable.
1. Non-Modifiable Risk Factors
These are factors that cannot be changed:
- Age: Risk increases significantly after 65.
- Sex: Slightly higher risk in men at younger ages. Women are more affected later due to longer life expectancy
- Genetics: Family history of stroke, heart disease, or rare conditions like CADASIL increases risk
- Previous stroke: A major predictor of future vascular dementia
2. Modifiable Risk Factors
These can be controlled or improved to reduce risk:
- High blood pressure (most important factor).
- Diabetes and high cholesterol.
- Smoking and obesity.
- Physical inactivity and poor diet.
- Heart conditions like atrial fibrillation.
- Sleep apnea and depression.
- Low cognitive stimulation and social isolation.
Many of these risks are interconnected… Well, if you manage them together is more effective than treating them separately.
Living with Vascular Dementia

A diagnosis of vascular dementia can be challenging… but with proper care, individuals can still maintain a quality of life for years.
For patients:
→ Structured routines and memory aids: To help with daily functioning!
→ Regular physical activity and social engagement: To support brain health!
→ Safety adaptations at home and advanced care planning are important in the early stages
For caregivers:
→ Understanding symptoms like anger or confusion as part of the disease is essential.
→ Caregiver support, respite care, and education reduce stress.
→ Early planning for long-term care and legal/financial decisions is important…
Get Cognitive Health Support with a Dementia Care Specialist in Florida!

Health & Psychiatry offers specialized dementia services, including dementia care specialists in Florida, who provide diagnosis, treatment, and ongoing support for both patients and families.
Early intervention and coordinated care can significantly improve outcomes and help manage vascular cognitive impairment more effectively.
Book an appointment to know your treatment options and step forward for a better health!
FAQs
What are the early signs of vascular dementia?
Early signs of vascular dementia include slowed thinking. Also, difficulty concentrating, trouble planning, and mild confusion. Mood changes like irritability, anger or depression may also appear.
Is vascular dementia reversible?
No. It is not. Vascular dementia irreversible. But its progression can often be slowed. It can be done by controlling risk factors like blood pressure, diabetes, and cholesterol.
What is the difference between vascular dementia and Alzheimer’s?
Vascular dementia is mainly caused by brain blood flow reduction. Often progresses in steps. While Alzheimer’s is caused by protein buildup and declines gradually.
Is vascular dementia hereditary?
Most cases are not inherited. But your family history of stroke or heart disease can increase risk. Also, rare genetic conditions like CADASIL can directly cause it.